Trigeminal neuralgia, often called TN, brings sharp, stabbing pain to the face. Many people wonder what can be mistaken for trigeminal neuralgia. This question matters because wrong diagnoses lead to delayed relief. In this guide, we explore conditions that mimic TN. We draw from trusted sources to help you understand and act. TN affects the trigeminal nerve, which sends sensations from the face to the brain. Pain hits suddenly, like an electric shock. It lasts seconds to minutes. Triggers include brushing teeth or a light breeze. But other issues cause similar pain, leading to confusion.
Experts estimate TN impacts about 12 in 100,000 people each year. Women over 50 face higher risks. Multiple sclerosis links to 1-2% of cases. High blood pressure and smoking raise chances too. Accurate diagnosis starts with your story. Doctors check pain type, location, and triggers. They use MRI scans to spot causes like blood vessel pressure or tumors.
Misdiagnosis happens often. One study shows up to 40% of TN cases first get labeled as dental problems. Patients endure needless root canals or extractions. This delays proper care. We aim to clear up these mix-ups. Read on for details on common mimics, how to spot differences, and steps for relief.
Understanding Trigeminal Neuralgia Basics
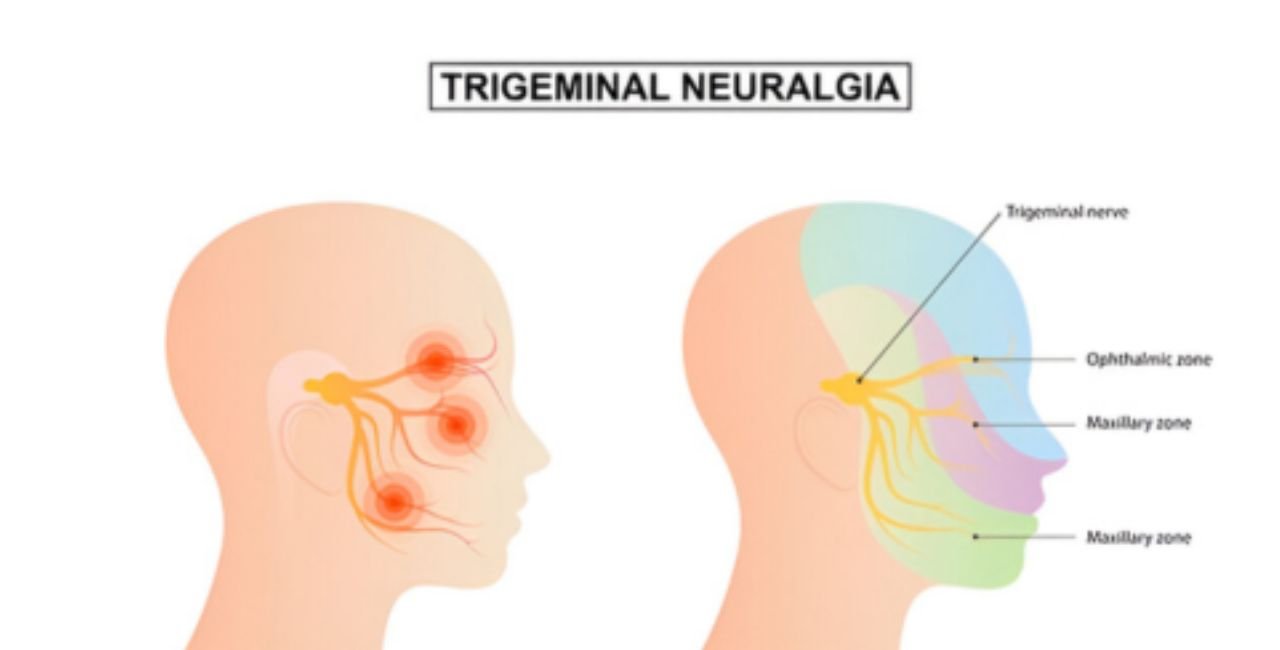
Before diving into mimics, grasp TN fundamentals. The trigeminal nerve has three branches: ophthalmic (eyes), maxillary (cheeks), and mandibular (jaw). Pain usually strikes one side. It feels intense, like a jolt. Episodes build over time.
Causes include:
- Vascular compression: A blood vessel presses the nerve, wearing down its protective sheath.
- Multiple sclerosis: Demyelination harms nerve signals.
- Tumors or cysts: Rare, but they compress the nerve.
- Trauma: Injuries from accidents or surgery.
Symptoms stand out:
- Sudden, severe pain.
- Triggers from everyday actions.
- Pain-free periods between attacks.
Living with TN challenges daily life. Simple tasks like eating or talking spark agony. Anxiety grows from fear of the next episode. But hope exists. Treatments range from meds to surgery. Early, correct diagnosis speeds recovery.
What Can Be Mistaken for Trigeminal Neuralgia: Common Conditions
Many conditions share TN’s facial pain. This section breaks them down. We highlight symptoms, differences, and why mix-ups occur. Bold key terms for clarity.
Dental Problems: A Frequent Mix-Up
Dental issues top the list of what can be mistaken for trigeminal neuralgia. Toothaches, abscesses, or cracked teeth cause throbbing jaw pain. This mimics TN’s lower face attacks.
Symptoms of dental problems:
- Constant ache, not sudden shocks.
- Swelling or sensitivity to hot/cold.
- Pain worsens with biting.
Differences from TN:
- TN pain bursts briefly; dental pain lingers.
- Touch triggers TN, but pressure affects dental issues.
- No nerve involvement in pure dental cases.
Why the confusion? Pain radiates to similar areas. One report notes 20-30% of TN patients first see dentists. They undergo procedures like fillings without relief. An exam or X-ray spots dental causes. If pain persists post-treatment, suspect TN.
Tips to differentiate:
- Track pain patterns. Note duration and triggers.
- Visit a dentist first for oral checks.
- If no dental fix helps, consult a neurologist.
For more on pain management, check Laaster.
Temporomandibular Joint Disorders (TMJD)
TMJD affects the jaw joint. It ranks high in what can be mistaken for trigeminal neuralgia. Stress, grinding teeth, or arthritis cause it.
Symptoms of TMJD:
- Jaw clicking or popping.
- Pain when chewing or yawning.
- Headaches or earaches.
Differences from TN:
- TMJD pain is dull and achy; TN is sharp.
- Joint tenderness present in TMJD.
- No electric shock feel.
Misdiagnosis stems from overlapping jaw pain. A study in the Journal of Oral Rehabilitation found 15% of TMJD cases mimic neuralgias. Physical therapy or mouth guards treat TMJD. MRI or CT scans confirm joint issues.
Steps for clarity:
- Feel for jaw tenderness.
- Note if pain ties to movement.
- Seek a TMJ specialist if symptoms match.
Sinus Infections and Their Role
Sinusitis inflames facial cavities. It often confuses with TN due to cheek and forehead pain.
Symptoms of sinus infections:
- Nasal congestion and discharge.
- Pressure behind eyes.
- Fever or fatigue.
Differences from TN:
- Sinus pain is steady pressure; TN is episodic.
- Accompanies cold symptoms.
- Improves with antibiotics.
About 10% of facial pain cases link to sinuses, per ENT reports. Triggers like allergies worsen it. CT scans show inflammation. Decongestants provide quick relief, unlike TN meds.
Actionable advice:
- Monitor for respiratory signs.
- Use saline rinses for relief.
- See an ENT if pain spreads.
Cluster Headaches: Intense but Distinct
Cluster headaches cause severe pain around one eye. They mimic TN’s unilateral attacks.
Symptoms of cluster headaches:
- Burning or piercing pain.
- Eye tearing or redness.
- Attacks last 15-180 minutes.
Differences from TN:
- Cycles in patterns (daily for weeks).
- Autonomic symptoms like runny nose.
- No touch triggers.
Men face higher risks. Smokers too. Prevalence: 1 in 1,000 people. Oxygen therapy or triptans treat them. According to Johns Hopkins Medicine, detailed histories separate them.
Differentiation tips:
- Note episode length.
- Check for eye changes.
- Track frequency cycles.
Postherpetic Neuralgia Following Shingles
Shingles damages nerves, leading to postherpetic neuralgia (PHN). It shares burning pain with TN.
Symptoms of PHN:
- Constant burn or itch.
- Skin sensitivity.
- Rash history.
Differences from TN:
- Follows shingles outbreak.
- Pain persists months.
- No brief shocks.
Over 50s with weak immunity risk it. Vaccine reduces chances by 50%. Antivirals treat early; lidocaine patches soothe later. Mayo Clinic notes MRI rules out other causes.
Steps to identify:
- Recall recent rashes.
- Test skin touch response.
- Vaccinate preventively.
Glossopharyngeal Neuralgia: Throat-Focused Pain
This affects the glossopharyngeal nerve. Pain hits throat, tongue, or ear.
Symptoms:
- Sharp jabs on swallowing.
- Ear or neck radiation.
- Coughing triggers.
Differences:
- Location: Back of throat vs face.
- Triggers: Swallowing vs facial touch.
- Rarer than TN.
Linked to aging or tumors. Surgery like microvascular decompression helps. Stats show it in 0.2-0.7 per 100,000.
Advice:
- Log swallow-related pain.
- Avoid acidic foods.
- Consult neurosurgeon.
Multiple Sclerosis and Nerve Damage
MS demyelates nerves, mimicking TN in 1-2% of cases.
Symptoms:
- Numbness or tingling.
- Vision issues.
- Fatigue.
Differences:
- Widespread symptoms.
- Progressive.
- MRI shows plaques.
Young adults affected. Meds like interferon manage. The Morrison Clinic stresses early scans.
Tips:
- Note body-wide signs.
- Get lumbar puncture if needed.
- Join support groups.
Migraines and Other Headaches
Migraines cause throbbing facial pain.
Symptoms:
- Nausea, light sensitivity.
- Aura precede.
- Last hours to days.
Differences:
- Pulsing vs stabbing.
- Bilateral often.
- No nerve-specific triggers.
Affects 12% of adults. Triptans treat. Lifestyle changes help.
Differentiate by:
- Aura presence.
- Duration.
- Family history.
Cervical Spine Issues
Neck problems like herniated discs compress nerves, radiating to face.
Symptoms:
- Neck stiffness.
- Arm weakness.
- Pain on turning head.
Differences:
- Originates from neck.
- Improves with posture.
- X-rays show.
Common in older adults. Physical therapy aids.
Steps:
- Assess neck mobility.
- Use heat packs.
- See orthopedist.
How Doctors Differentiate TN from Mimics
Diagnosis relies on history and exams. Bold steps include:
- Describe pain: Note intensity, duration, triggers.
- Physical exam: Touch face for sensitivity.
- Imaging: MRI spots compression or MS.
- Nerve tests: Rule out other neuropathies.
If unsure, trials of TN meds like carbamazepine help. Response confirms. Avoid unnecessary procedures.
Treatment Options for TN and Mimics
Once identified, treat accordingly.
For TN:
- Meds: Anticonvulsants first.
- Injections: Botox or nerve blocks.
- Surgery: MVD for lasting relief.
For mimics:
- Dental: Antibiotics or extractions.
- TMJD: Splints.
- Sinus: Decongestants.
Holistic approaches: Acupuncture, yoga reduce stress.
Living with Facial Pain: Tips and Strategies
Manage daily:
- Avoid triggers.
- Keep a pain diary.
- Use soft foods.
Support: Join groups for stories.
Statistics and Insights on Misdiagnosis
Misdiagnosis delays care by months. 30% face multiple dentist visits. Women: 58% of cases. Age 50+: 70%.
FAQs
What can be mistaken for trigeminal neuralgia? Common mimics include dental problems, TMJD, sinus infections, cluster headaches, PHN, glossopharyngeal neuralgia, MS, migraines, and cervical issues.
How do I know if it’s TN or something else? Track symptoms. See specialists for exams and scans.
What triggers TN pain? Light touch, eating, wind.
Can TN be cured? Surgery offers long-term relief for many.
When to see a doctor? If pain disrupts life.
Conclusion
In summary, what can be mistaken for trigeminal neuralgia includes dental issues, TMJD, sinus infections, cluster headaches, and more. Each shares facial pain but differs in triggers and patterns. Accurate diagnosis through history, exams, and imaging brings relief. Treatments vary from meds to surgery. Stay informed and seek help early. This reduces suffering and improves life.
What facial pain have you experienced, and how did you address it?
References
- The Morrison Clinic. “What Can Be Mistaken for Trigeminal Neuralgia.” Accessed January 2026. Provides clinic insights on mimics and treatments for patients seeking neurosurgical options.
- Johns Hopkins Medicine. “Trigeminal Neuralgia.” Accessed January 2026. Offers authoritative details on causes and surgeries for those with severe facial pain.
- Mayo Clinic. “Trigeminal Neuralgia – Diagnosis and Treatment.” Accessed January 2026. Details diagnostic steps and meds for general audiences exploring options.


